Research In Action
Research In Action
Breadcrumb
In the field of pediatric concussion, we have made tremendous progress in the management of injury the past two decades. Historically, concussion management was focused on passive rest, recommended in a one-size-fits-all fashion. Based on evidence generated by our researchers and through our multidisciplinary clinical team in the Minds Matter Concussion Program, that management strategy has shifted to a much more active and individualized approach. We have found that personalized rehabilitative therapies, delivered in a fashion targeted to a patient’s signs and symptoms, significantly accelerate recovery.
One key issue is that these proven therapies are primarily prescribed and recommended by concussion specialists, yet we have shown nearly all pediatric concussion patients are first diagnosed outside of the specialty setting. In fact, the journey from injury through specialty care completion contains multiple steps; this presents multiple junctures at which a patient might “fall off” the care pathway or encounter barriers to receiving optimal care. This phenomenon is known as a “leaky pipeline”.
In a study recently published in the Journal of Pediatrics, we assembled a multidisciplinary team of clinicians and scientists, including Tyra Bryant-Stephens, MD, Children’s Hospital of Philadelphia (CHOP) Chief Health Equity Officer and Associate Vice President, and Sadiqa Kendi, MD, MPH, the Chief Medical Officer of Safe Kids Worldwide and Associate Division Chief for Children’s National Medical Center Division of Emergency Medicine. We applied the rigorous structure of the Injury Equity Framework, co-developed by Dr. Kendi, and used CHOP’s Minds Matter Registry, unique in its scope, size, and depth, to ask the question of what disparities exist at the following three critical junctures in the pipeline of pediatric patients who sustained head trauma:
- Emergency department (ED) diagnosis of concussion
- Referral to concussion specialists after diagnosis
- Attendance of at least one specialty visit after referral
There are clear and distinct takeaways. Of the 22,344 patients less than 18 years of age evaluated for head trauma in the CHOP EDs between 2018 and 2025, we found:
- 5998 (27%) were diagnosed with concussion
- 142 of those diagnosed (19%) were referred to specialty care
- 487 (43%) of those referred attended at least one specialty visit.
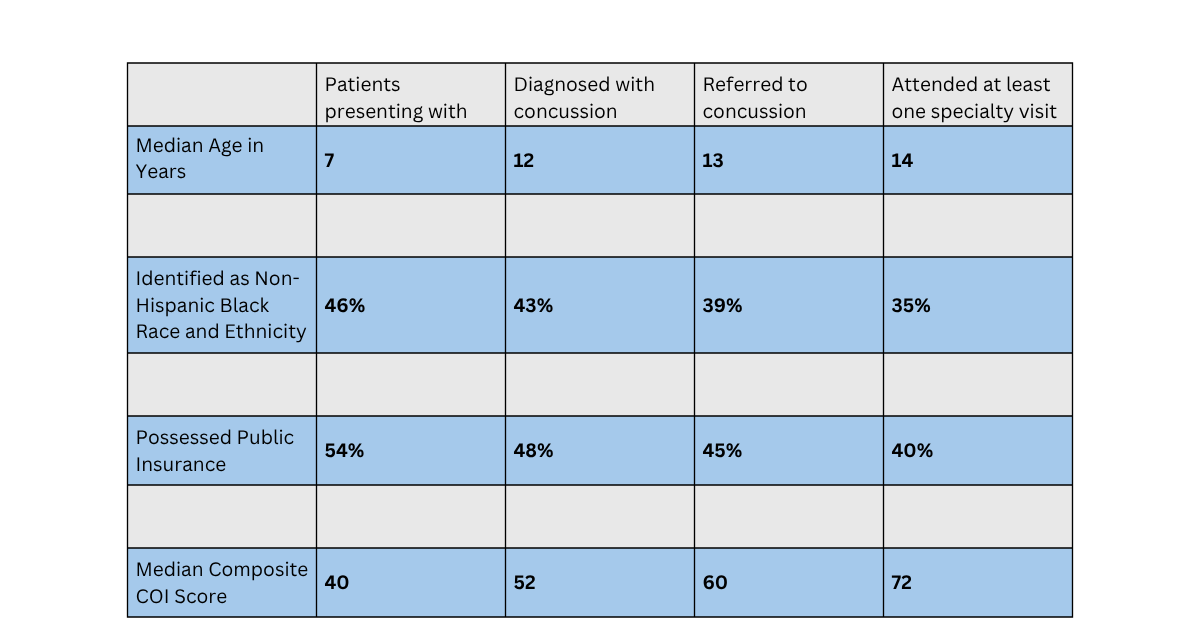
At these three critical junctures, we found the following differences across four key sociodemographic variables, including median age, race and ethnicity, insurance status, and the Child Opportunity Index (COI), a metric that combines 44 different indicators important to the growth and development of children at the neighborhood level, scaled from 0=least opportunity, to 100=most opportunity:
These results tell us that disparities in access to concussion specialists are driven by multiple factors, and a single intervention to improve care equity is unlikely to be sufficient. However, they can be used as a guide to target interventions to reduce these disparities and improve care equity. Specifically, in the Minds Matter Program, we have been a leader in this space in two broad areas: changing the way our clinicians interact with our patients (diagnosis and referral) and changing the way our patients interact with the healthcare system (follow-up and visit attendance).
Over the past decade, we have implemented electronic clinical decision support tools across diverse care settings, including primary care and the emergency department, with significant success. These are focused on bringing specialty evaluation maneuvers, such as visio-vestibular examination (VVE) testing, into the hands of our front-line clinicians to aid in concussion diagnosis. Starting in 2023, we launched a study of a novel clinical decision support tool that can go beyond diagnosis, aiding in guiding specialty referral in an objective fashion, to six of our primary care network sites. We hope this tool will improve care for all our care network patients, with a specific lens on those evaluated in urban practices. That study is wrapping up this spring, and we are excited to begin analyzing the results to share with other primary care sites across the CHOP network and the country.
We have also made significant efforts to boost our use of remote management tools to help patients and their families navigate the concussion journey between, and even before, traditional in-person follow-up visits. We have demonstrated the feasibility of using remote monitoring to track concussion symptoms in patients from diverse care settings, including for ED patients, and are currently exploring the use of similar technology, integrated in the patient’s electronic health record, to deliver targeted therapeutic recommendations and facilitate specialty care access. This work is part of a broader effort within CHOP’s digital health team to bring remote patient management into the hands of our diverse patient population. We also anticipate wrapping up that study later this spring and look forward to analyzing those results to continue to build on this critical work.
Ultimately, Minds Matter remains committed to improving care equity for our pediatric concussion patients, ensuring all patients have access to the most up-to-date, evidenced-based therapeutic approaches that can most expedite recovery and return to pre-injury baseline activities.